- Education
- Research
- Transplant Oncology Infectious Diseases Program
Our fellows see inpatients at three institutions: NewYork-Presbyterian/Weill Cornell Medical Center (NYP/Weill Cornell), Hospital for Special Surgery (HSS), and Memorial Sloan-Kettering Cancer Center (MSKCC).
NewYork-Presbyterian /Weill Cornell Medical Center (NYP/Weill Cornell Medicine) is the primary institution of our fellowship training program. The medical center is located in a large clinical and research complex on the Upper East Side of Manhattan. It is the the product of a merger of two distinct institutions with great history: the New York Hospital (founded 1771, affiliated with Weill Cornell Medical College since 1898) and, Columbia-Presbyterian Medical Center (founded 1868, affiliated with Columbia University Irving Medical Center since 1910). Presently, NewYork-Presbyterian Hospital (NYPH) is the largest health care facility in the New York metropolitan area, and one of the largest and most prestigious in the world.
The Greenberg Pavilion of NYP/Weill Cornell Medicine is a one million square foot facility with 800 inpatient beds. The hospital serves patients with a broad range of socioeconomic and cultural backgrounds, reflecting the diversity of New York City. NYP/Weill Cornell Medicine provides an extensive assortment of services through its Level I Trauma Center, Comprehensive Cancer Center, Burn Center, Bone Marrow and Blood Stem Cell Transplant Program, surgical services including neurosurgery and solid organ transplantation, and OB-GYN, pediatric, neurologic, and psychiatric departments. Fellows learn to manage patients infectious diseases ranging from common to rate in a myriad of medical settings.
At NYP/Weill Cornell Medicine, fellows rotate on our General ID consult service, as well as the Transplant Oncology Infectious Diseases service (leukemia, lymphoma, solid organ, and stem cell transplant). The General ID consult service includes exposure to inpatient HIV care and opportunistic infection management. First-year fellows spend ~10 months on clinical rotations (including electives) and second-year fellows spend ~2 months. Fellows are supervised 1:1 by an ID faculty member. In addition, ID PharmD.'s round daily with the General ID consult team providing invaluable education regarding the appropriate use and monitoring of antimicrobials. Other trainees, including medical students and residents (both medical and surgical subspecialty) are integrated into the consult team providing our fellows wonderful clinical teaching experience.
NYP/Weill Cornell Medicine is physically connected to our affiliate, Hospital for Special Surgery (HSS), a ~200-bed orthopedic hospital. HSS provides specialized surgical and rheumatologic care. Its independent ID division has unique expertise in bone and joint infections and their faculty have joint appointments at Weill Cornell. This affiliation offers our fellows unparalleled exposure to infectious diseases of the musculoskeletal system.
Memorial Sloan Kettering Cancer Center (MSKCC), located across the street from NYP/Weill Cornell, is a 500-bed hospital specializing in evaluation and treatment of oncologic conditions and is a designated National Cancer Institute Comprehensive Cancer Center. MSKCC offers our fellows a unique opportunity to learn about infections in the severely immunocompromised host in a highly specialized institution. MSKCC has their own ID fellowship, and their fellows rotate on our NYPH/Weill Cornell in-patient service in a reciprocal fashion. A combined Trans York NewYork-Presbyterian Hospital/MSKCC Infectious Disease clinical case conference is held regularly and both groups of fellows jointly attend the summer series of core topics in ID at the beginning of each academic year.
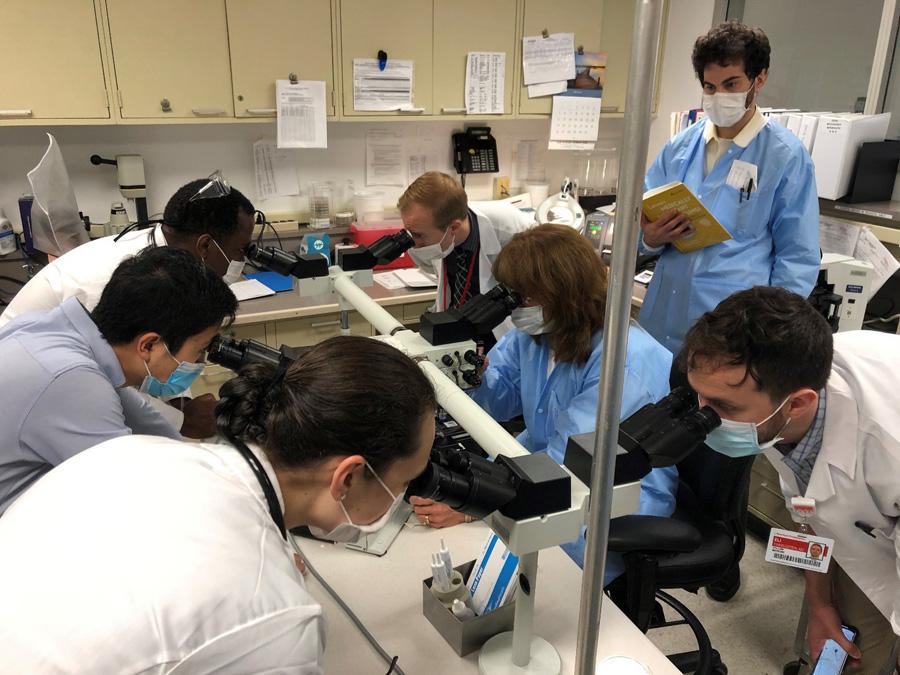
Fellows spend two weeks in in our Clinical Microbiology laboratory, which is led by Dr. Lars Westblade (Director) and their Associate Directors, Drs. Jamie Marino and Jefrrey Kubiak. The laboratory performs ~500,000 procedures each year and is a major reference laboratory serving the New York metropolitan area. Fellows will learn how to diagnose bacterial, mycobacterial, viral, fungal, and parasitic diseases. Molecular testing is the most rapidly expanding portion of the laboratory and is incorporated in many areas (e.g., diagnosis of bloodstream infection, meningitis/encephalitis, gastrointestinal disease, respiratory tract infection, sexually transmitted infection, and myocarbial infections). A major research interest of the laboratory is the implementation and evaluation of assays and algorithms for infectious diseases diagnostics and their impact on clinical as well as overall costs.
During the first two years, our fellows have weekly half-day continuity clinic sessions at the Center for Special Studies (CSS) HIV clinics and in ID Associates (general ID clinic) to evaluate new patients referred from the community as well as provide continuity outpatient care for patients seen on the inpatient service. Fellows gain expertise in the longitudinal care of patients with infectious diseases including HIV/AIDS, as well as outpatient antibiotic management.
Fellows may also rotate in our Travel Clinic, where they can learn about pre- and post-travel advice including malaria prophylaxis and travel-specific immunizations. Finally, interested fellows may also obtain experience in the management of sexually transmitted diseases through a rotation at the New York City Department of Health Bureau of Sexual Transmitted Infection clinics.
Subspecialty elective-rotations (two to four weeks at a time) are available to our fellows. These rotations provide them with more intense and dedicated exposure to specific types of infections. The rotations are staffed by senior clinicians with specific clinical expertise/research interests in that area. Current electives include:
Fellows interested in global health also have the option of an international elective at Weill Bugando Medical Center in Tanzania or other sites coordinated by Cornell University's Center for Global Health.
During the first two years, our fellows have weekly half-day continuity clinic sessions at the Center for Special Studies (CSS) HIV clinics and in ID Associates (general ID clinic) to evaluate new patients referred from the community for common outpatient ID problems as well as provide continuity outpatient care for patients seen on the inpatient service. Fellows gain expertise in the longitudinal care of patients with infectious diseases including HIV/AIDS, as well as in outpatient antibiotic management including OPAT (Outpatient Parenteral Antimicrobial Therapy).
Fellows may also rotate in our Travel Clinic, where they can learn about pre- and post-travel advice including malaria prophylaxis and travel-specific immunizations. Finally, interested fellows may also gain additional experience in the management of sexually transmitted diseases through a rotation at the New York City Department of Health Bureau of Sexual Transmitted Infection clinics.
| Rotation | First Year | Second Year |
|---|---|---|
| General ID consult service | 24-26 weeks | 6 weeks |
| Transplant Oncology ID | 6-8 weeks | 2 weeks |
| Clinical electives | 4 weeks | Optional |
| Memorial Sloan-Kettering | 4 weeks | Optional |
| Hospital epidemiology | 2 weeks | Optional |
| Microbiology | 2 weeks | Optional |
| Research | 4 weeks | 40 weeks |
| Vacation | 4 weeks | 4 weeks |
| Rotation | First Year | Second Year |
|---|---|---|
| General ID consult service | 26 weeks | 6 weeks |
| Transplant Oncology ID | 6 weeks | 2 weeks |
| Clinical electives | 4 weeks | Optional |
| Memorial Sloan-Kettering | 4 weeks | Optional |
| Hospital epidemiology | 2 weeks | Optional |
| Microbiology | 2 weeks | Optional |
| Research | 4 weeks | 40 weeks |
| Vacation | 4 weeks | 4 weeks |